A Hepatic Artery Infusion Pump Keeps Colorectal Cancer in Check
contributed by Ian Demsky; originally appeared on the Michigan Medicine Health Blog
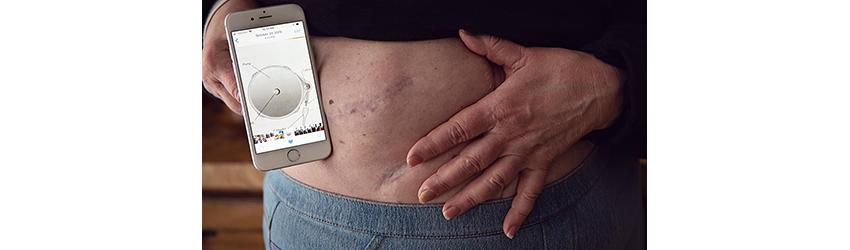
This decades-old tool has helped keep Ellen Hoff's Colorectal Cancer in Check

Photos by Leisa Thompson
For more than 25 years, Ellen Hoff has helped keep things running at the General Motors Proving Ground in Milford, Michigan.
“When equipment goes down, it’s my responsibility to get replacement parts there yesterday,” she says.
Her can-do attitude and attention to detail also served her well during her days as a NASCAR crew member, scoring for a racing team based in Holly.
“For those years, I spent more time in the air and on the road than I did at home,” adds Hoff, 57, of Ortonville. “Generally, I would work three to four days a week and be gone every Friday through Monday.”
But in 2016, she experienced some serious setbacks.
First, in August came the death of her brother, whom she calls her “best friend.” And then in October she was diagnosed with stage 4 colorectal cancer, meaning it had already spread to her liver.
“After my colonoscopy, the doctor came out and very directly told me, ‘You have cancer.’ Just that immediate.”
Hoff met with a multidisciplinary care team at the University of Michigan Rogel Cancer Center and they came up with a plan. She would undergo an operation to remove both the cancer in her large intestine and the three tumors starting to grow on the surface of her liver. Oncologist John C. Krauss, M.D., the medical director of the Multidisciplinary Colorectal Cancer Clinic, would coordinate her care through successive rounds of chemotherapy.
My doctors were great, Hoff says of Krauss, her colorectal surgeon Karin Hardiman, M.D. (now at the University of Alabama at Birmingham), and her liver surgeon Clifford Cho, M.D.
“They told me, ‘We’re pretty confident we can get it all.’ The tumors on the liver were just on the surface and they were small. They made me feel like, ‘Hey, we’ve got this.’”
Over that next year, follow-up scans showed Hoff remained cancer free. But then in April 2018, an MRI revealed a new spot on her liver.
She underwent a second operation on her liver to remove the metastasis. And then six months later, a third operation. And in September 2019, a fourth. The tumors in her liver just kept coming back.
It was during that fourth operation that Cho implanted a device known as a hepatic artery infusion pump, designed to deliver powerful chemotherapy directly to her liver.
“The pump is an acknowledgement that if you have someone whose cancer keeps coming back after surgery, it’s going to happen again,” Cho says. “It allows us to be much more aggressive in delivering chemotherapy directly into the liver — which in Ellen’s case, was the place where her body and her cancer demonstrated she was most likely to have a recurrence.”
Technology developed at U-M
Use of the pump, which is about the size and shape of a hockey puck, was actually developed at Michigan in the late 1970s and early 1980s by William Ensminger, M.D., Ph.D., and his colleagues.
“It’s not a cure, but it represents the most effective means of regressing tumors residing in the liver,” Ensminger says in a 1981 UPI wire story that was picked up by The New York Times. “It is a major breakthrough.”
Because the liver is so good at breaking down the powerful chemotherapy agent fluorodeoxyuridine, or FUDR, it can be delivered at levels that would be overwhelmingly toxic if given throughout the whole body like most chemotherapies, explains Ensminger, an emeritus professor of pharmacology.
“The pumps used to be so scarce, my wife and I would drive out to the airport to pick them up so they could be implanted the next day,” he recalls.
Patients came from across the country to receive this cutting-edge advancement (moreover, Ensminger worked with the device’s manufacturer to adapt the concept into today’s well-known chemotherapy infusion ports.)
But as new and better general chemotherapy drugs were developed, and more aggressive surgical techniques adopted, use of hepatic artery infusion pumps started to fall out of favor at many health systems, including at U-M.
And while their adoption was never widespread, the evidence of their efficacy has been “quite compelling,” leading some places to give them a fresh look, notes Cho.
A 2017 study published in the Journal of Clinical Oncology, for example, examined 20 years’ worth of patient data, finding those who received the pumps tended to live two years longer than their peers who did not.
Their use at Michigan was discontinued for a time until surgeon Hari Nathan, M.D., Ph.D., helped to restart the program in 2018. Since then, about 35 patients have received one.
“As far as technology goes, they’re an oldie but a goodie,” Nathan says. “I think of the pump as one tool in a big toolbox that we can offer to patients with colon and rectal cancer. If you look at the whole toolbox, it would include systemic chemotherapies, regional chemotherapies like the pump and HIPEC — which involves putting chemotherapy into the body cavity ‐ various ablation techniques, and radiation therapy.
“With such a robust armamentarium, we at the Rogel Cancer Center can really select the individual tools and techniques that are going to be best for each patient,” he adds.
‘Not any big deal at all’
Hoff calls her pump a “godsend.”
“At first it was very intimidating, but it was really not any big deal at all,” she says. “I’ve had no pain, no problems.” Since the pump delivers chemotherapy directly to her liver, it didn’t cause the unwelcome side-effects that accompanied her earlier rounds of full-body chemotherapy.
Today, rather than chemo, her pump is filled with blood thinner and saline solution to keep it clean and working in case she needs additional treatment in the future. She visits the U-M clinic once a month to have it filled.
“Ellen was having tumor recurrence every six to nine months before we placed the pump. And since then she’s gone longer than ever before without a recurrence — about a year and a half,” Krauss says. “I call that a home run for the pump.”
The liver has a complex blood flow with two inputs — the hepatic artery and the portal vein ‐ and only one output. Tumors that grow in the liver tend to get their blood supply from the hepatic artery, which allows the chemo to travel from the pump directly to them.
“This unique blood flow is one of things that makes the pump work,” notes Krauss. “We can’t do it in the lungs. We can’t do it in the kidneys.”
It also means that patients whose cancer has spread significantly beyond the liver aren’t good candidates for the pump.
Advice for other patients
Hoff says her Christian faith and her friends from church have been important sources of comfort and solace throughout her cancer journey.

“When someone tells you that you have stage 4 cancer, at first it’s overwhelming,” she says. “But after you start working with your doctors, it becomes a little more manageable. You say, OK, now I think I understand a little better. They’re telling me that this is what we’re going to do next and this is what we’re going to try, and if that doesn’t work, we’re going to try something else.”
Her team at Michigan Medicine helped her to persevere through the challenges of hearing again and again that her cancer had returned.
“You just take one step at a time,” she says. “Take the encouragement you get from them. They make you feel more at ease. They said to me: We’re going to get through this. We’re going to do everything we can to make this better. So they’ve always been very encouraging.”
Last year, the arrival of the coronavirus presented new challenges for most Americans, and Hoff was no exception. She hasn’t been able to hug her mother, who is almost 90, since the pandemic started and many of their visits have to be conducted through a closed glass door. Cancer also claimed several close friends, she says.
“It was definitely a huge, huge challenging year,” Hoff says. “But although the year was really, really rough, my biggest thing is that I pray for the people who have lost their jobs, lost their homes, can’t feed their families. Those are the people that really need help right now. Compared to many, I’m doing pretty well.”
Learn more about advanced cancer and innovative cancer treatment:
