Coping with COVID and then cancer
contributed by Anna Megdell
Andrew Ackerman was the first COVID-19 patient to be treated with an experimental filter that reduced his inflammation, helping to save his life. During treatment, lung cancer was discovered.
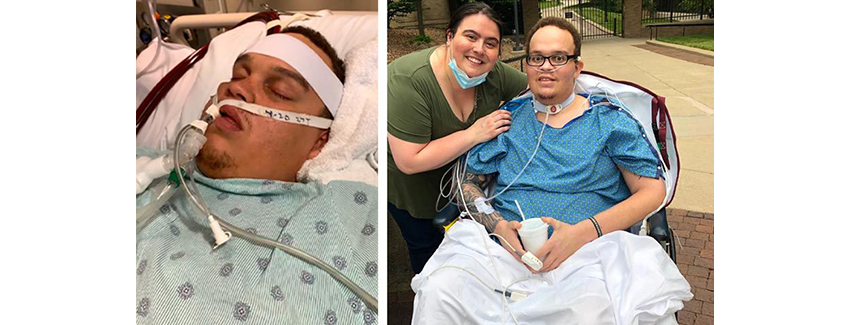
Photos courtesy Andrew Ackerman
In April 2020, 26-year-old Andrew Ackerman couldn't seem to kick a bad sinus infection. Providers at an urgent care told him he just needed some sleep.
But, a week into his symptoms, he was so tired he couldn't make it from the bedroom to the front door of his house without collapsing. His girlfriend, Elizabeth, had to call 911 just to get Andrew to a local hospital. After six days with no improvement, he was transferred to Michigan Medicine, where more resources were available to help him.
Andrew would go on to spend 75 days at Michigan Medicine’s University Hospital due to acute respiratory distress syndrome from severe COVID. He’d return to U-M for follow up visits to address complications for more than a year afterward.
“I went from being healthy to virtually being on my deathbed in a matter of days,” Andrew said.
"We didn't think COVID was a thing that we had to worry about because we're young and we're not our grandparents and we don't have preexisting conditions," Elizabeth said. "We were convinced things like this don't happen to people like us. But we were wrong, and here we are."
The filter that could
When an ambulance arrived at Andrew’s house, his oxygen levels were so low that they didn’t register on an oximeter. The second time paramedics tried to measure his oxygen saturation, it was 56%. Normal levels typically range between 95 and 100%.<
By the time Andrew got to Michigan Medicine, he was in septic shock, resulting in organ failure and very low blood pressure.
The providers tried everything to help Andrew recover.
“We used every therapy we had possible for him, including ECMO,” said Lena Napolitano, M.D., the director of surgical critical care at University of Michigan Health and the Massey Foundation Professor of Surgery at the University of Michigan Medical School.
ECMO is a form of life support that manually adds oxygen and removes carbon dioxide from the blood, giving a patient’s heart and lungs a break from their typical responsibilities so their body can heal. Robert H. Bartlett, a U-M professor emeritus of general surgery, led the development of ECMO back in the 1980s, and the technique has saved the lives of many patients with COVID at U-M Health and beyond during the pandemic.
But even ECMO wasn’t working for Andrew.
“We weren’t making progress in getting his lungs to start to function again,” Napolitano said. “We thought he had excessive inflammation, which makes your lungs work poorly. Picture slapping your hand against a wall. It would end up all inflamed and swollen, right? His lungs were like that. We had to get rid of that before his lungs could oxygenate well.”
Visitors weren’t allowed at the hospital, so Napolitano updated his parents and girlfriend twice a day by phone.
“For two months, we were just waiting for the phone to ring,” Elizabeth said.
The breakthrough came when Napolitano and her team partnered with the division of nephrology, which had recently developed a filter to remove compounds causing inflammation in the lungs and kidneys. While Andrew lay in a hospital bed, unaware of what was happening around him, his parents gave permission for him to be the first patient with COVID to be treated with the experimental device.
Within 52 hours, Andrew improved significantly. A clinical trial is now studying the technology for use in COVID patients.
“This is a great example of how we pull out every stop, every treatment strategy possible to try to save the lives of those with COVID,” Napolitano said. “It’s not a quick road. It’s not one therapy. It’s a lot of therapies and the whole intensive care unit team managing them every single day.”
Starting to recover
Andrew needed to remain on the newfangled device for 17 days. Once he was taken off of both it and ECMO, he began breathing on his own, through a tube in his trachea.
“I remember him being big-eyed, with a deer-in-the-headlights look,” said Kelli Marino, R.N., who was one of Andrew’s nurses. “He was understandably nervous and lonely. That was a time when families weren’t allowed to come in. The nurse that had him on Mother’s Day worked to get his sedation down, so he could be a little more interactive and FaceTime with his mom.”
Another month passed before providers were able to take Andrew’s breathing tube out, and he started inpatient rehab shortly afterward.
“He was definitely confined more with a leg brace and a wheelchair at the beginning,” Marino said. “But he just kept going with the physical therapy and pushing through. His momentum to keep going was great to see.”
“Many of our patients who have been sick for so long are sick and tired of being ill and don’t want to put forth all the effort for physical therapy that is really hard,” Napolitano said. “But Andrew was full-court press. We asked him to take deep breaths 10 times every hour, and he was ready and willing to do it. It was amazing that we got to see that part of him — how stoic he was, how strong he was, how motivated he was to get his life back.”
And, on July 3, 2020, Andrew Ackerman was able to go home.
Finding — and removing — cancer
Andrew faced severe complications to overcome: deconditioned legs, poorly functioning kidneys, bleeding into his muscles that kept him from walking properly.
“COVID doesn’t just stop once your test is negative,” Elizabeth said. “There’s a lot of stuff that still happens after that.”
When Napolitano and team did a CT scan of Andrew’s lungs to check for blood clots, they found clots, yes, but also a large tumor in his chest — one that might not have been identified without his hospitalization for COVID.
But, given Andrew’s continued recovery, the mass couldn’t be removed immediately.
“When he came to us, he was in bad shape,” said Elliot Wakeam, M.D., a thoracic surgeon and assistant professor at Michigan Medicine. “He had no hair. He looked not well. We had some CAT scans from when he was in the hospital, and we had an idea that the mass wasn’t growing that much. We figured the best way to balance the risk was to wait and let him get better from his COVID and hospitalization and delay the surgery.”
Wakeam followed Andrew’s progress for a while, watching as Andrew recovered “amazingly” well from his bout with COVID. In spring of 2021, Wakeam was able to completely remove the mass.
“Andrew continues to get scans every four to six months to ensure the tumor hasn’t returned,” Wakeam said. “But he’s now essentially considered cured. Beyond dodging a massive bullet in the form of horrible COVID, he dodged a bullet here, too.”
Trusting the ‘lady who saved Andrew’s life’
When COVID-19 vaccines became available, Andrew and Elizabeth turned to Napolitano for guidance — unintentionally, at first.
Napolitano was one of five frontline workers whom Michigan Medicine had selected at random to get the first shots of the vaccine at the health system. She was featured in a video documenting that day that Elizabeth saw on Instagram.
Elizabeth said she shared the video with everyone she knew.
"This lady saved Andrew's life," Elizabeth said. "If she knows how to save someone's life who shouldn't have gotten sick in the first place but did, and she's getting the vaccine, then why wouldn't we get it? It just made sense."
"I knew they were filming it, but I didn’t know it was going to be everywhere, so I didn’t tell anybody," Napolitano says. "What I intentionally did is every one of our patients that came back to clinic, including Andrew, I was begging them to be vaccinated. Yes, we were able to get Andrew through, but it’s much better if you never get that sick. I always say I wish I could grab every unvaccinated person in the world and walk them through our intensive care unit to see young, healthy people on life support not doing well.”

Kendra Koman with Kendra Koman Photography
The best outcome
Andrew has, as Napolitano said "been through hell, the poor guy."
"But," she added. "His girlfriend was there the whole time."
“There are some days where I get that ‘Woe is me’ type thing,” Andrew. “Then I take a step back, and I think, ‘You’re here. You have to be patient.’ Elizabeth has been huge being there every step of the way. If I didn’t have her, I think it’d be a completely different situation.”
He paused and thought back to the beginning of his relationship.
"When I first got in the hospital, Elizabeth and I were still new at dating," he said. "Waking up, I still couldn't talk and I remember seeing her face. She was still there when she had every opportunity to run, and she didn't. It was more than obvious, like a slap in the face, that she's the one, and I'm not letting her go."
“I like to think of myself as a planner,” Elizabeth said. “But I couldn’t plan for this. The biggest lesson from all of this was that life is short, and you have to take advantage of every minute that you can.”
Andrew proposed about two months after he was discharged from the hospital, at a winery in Traverse City, and he and Elizabeth got married on Oct. 30, 2021.
Instead of spending money on favors for their guests, they made a donation to the Michigan Medicine Surgical Intensive Care Unit. They shared this news at their reception, complete with a round of applause to honor health care workers and recognize what they’ve been through over the past few years.
"Those 75 days were very scary and filled with a lot of unknowns, but the U-M team helped us more than they will know," Elizabeth wrote in an email to U-M’s development office. "They are what inspired the gift from us. ‘Thank you’ will never feel like enough.”
Note: The experimental device was used in this patient under an emergency expanded access approval from the FDA. It is made by Seastar Medical, Inc., a company in which Michigan Medicine researcher H. David Humes, M.D., study coordinator Angela Westover and the University of Michigan hold a financial interest. The company also has a clinical trial of this approach under way at U-M and elsewhere; U-M’s participation in the trial is managed under all applicable U-M policies and overseen by Lenar Yessayan, M.D.
