Anatomy of a Visit
Behind the waiting room walls in the U-M Rogel Cancer Center
It's about 2:30 p.m. on a Tuesday, and the infusion pharmacy is buzzing as its staff hunkers down to get through the U-M Rogel Cancer Center's busiest day.

Pharmacist Diane Klemer breaks away -- as a pharmacist does every day about this time -- to huddle with nurses who coordinate each of the centers five infusion areas.
Klemer scans the list of 130 patients scheduled for infusion treatments the next day. Her goal is to troubleshoot bottlenecks and problems: Are there too many patients coming in at 7:30 and 8 a.m.? Have patients who receive carefully timed treatments been scheduled appropriately?
"We find that if we spend 10 to 15 minutes the day before with each infusion area, talking through the next day's schedule, we can address staff concerns, make corrections, if necessary, and provide better service the next day for our patients when they are here," said Kelly Wright, manager of the Rogel Cancer Centers Infusion Pharmacy.
Nothing about chemotherapy is simple, especially not for those patients who have to endure its side effects while relying on it to treat their cancers. But few patients ever see the more than 100 health-care professionals working through a complex series of checks and balances to ensure the 36,000 infusion treatments delivered each year at the Rogel Cancer Center are appropriate and safe.
This is the story of just one of those many treatments.
2:30 p.m., Tuesday
Twenty-four hours before treatment is scheduled to begin, Diane Klemer has spotted Barbara Friesen's name on the list of the next days patients. Klemer confers with Lynn Lamirand, the nurse coordinating the Med Inn Infusion Area that day, during a daily phone call. Friesen, an eight-year sarcoma survivor, is coming in for treatment she receives once every three weeks as part of a research study. Everything looks in order.
9:30 a.m., Wednesday
Friesen gets in her car for the 150-mile trek from her Berrien Springs home to the U-M Rogel Cancer Center. Because she lives so far away, her blood has already been tested at a facility near her home to make sure she is able to receive treatment.

Noon
Pharmacy technician Lisa Aunins fills an IV bag with saline solution that will be used to prepare Friesen's treatment. Although the pharmacy will not receive a prescription until Friesen has seen her physician, Aunins is getting a head start, shaving 15 minutes off of the time it will take to prepare the drug later.
1:30 p.m.
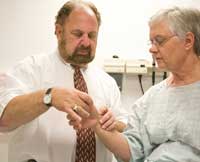
Having already checked Friesen's vital signs, medical assistant Amy Fardig escorts Friesen back to Exam Room 37. Nurse practitioner Denise Reinke enters about five minutes later and asks Friesen how she has been feeling since her last treatment. Friesen, a former physical education teacher who now works on special projects for Andrews University, says she's been working 12-hour days and feeling pretty good. "You can sit down and shrivel up or keep going," she says.
1:40 p.m.
Laurence Baker, D.O., examines Friesen and says her latest diagnostic scans look stable. Friesen asks a question about her level of monocytes -- a type of white blood cell -- and some swelling in her wrist.
"I think I'm doing well," Friesen says.
"Yeah, I think you are, too," Baker replies. "As long as we're in agreement."

1:55 p.m.
As Friesen leaves the clinic, nurse Diane Neelands faxes an order for Friesen's chemotherapy to both the Infusion Pharmacy and the Med Inn Infusion Area. Dr. Baker has already doublechecked the prescription Reinke wrote.
2:05 p.m.
Donald "Joe" Carter, an infusion pharmacist, receives the fax, checks the calculations and puts the order into the Cancer Center's computer system. He prints out a label and passes it along to Klemer, who re-checks all calculations and ensures the accuracy of the label.
2:14 p.m.
Friesen checks in at the Med Inn Infusion Area. The pharmacy will not begin work on the prescription until a nurse in the infusion area has verified that a patient is healthy enough to undergo treatment. One minute later, a nurse in the infusion area clicks a button on her computer; the message pops up in the pharmacy: "patient go."
2:20 p.m.

2:28 p.m.
Pavuk checks the calculations on the order and snaps off the light under the hood where she works to protect the lightsensitive drug. The hood's exhaust fan cleans the air of toxic fumes, and Pavuk wears a gown along with glasses and gloves to protect herself. She fits each of the vials with a special plastic top shaped like a miniature airhorn to prevent toxic chemicals from dripping. Needles and IV tubing are also fitted with specially designed plastic parts to prevent leaks. "All the pieces fit together like a jigsaw puzzle, so none of the liquid escapes," Pavuk says.
2:53 p.m.
Pavuk injects each vial with sterile water to dilute the drug and then drains each of the nine vials with a needle. She pops off the safety valve on one of the vials to squeeze out the last milliliter.
3:02 p.m.

Pavuk pushes a red button. Kelly Wright, Infusion Pharmacy manager, comes over to check her work: Is it the right drug? Are the vials right? Have they expired? What did Pavuk use to dilute the drug? Is the dilution amount right? Is the math correct? Only at this point does Wright turn to the hood to inspect the needle Pavuk has filled. After Wright checks the label and gives her the OK, Pavuk injects the drug into the prepared IV bag. The tech manipulates it to eliminate all air bubbles, which could cause Friesen's pump to shut down.
Pavuk slips the finished product into a brown plastic cover to protect it from light. Another tech sends a message to infusion: Time for pick-up.
3:21 p.m.
Medical assistant Deborah Rattai stops at the Infusion Pharmacy window to pick up the bag. She heads back to Med Inn Infusion, pausing outside the elevator to help a patient's wife and daughter find Big Bird in C.S. Mott Children's Hospital. "Oh, shes a doll," Rattai says of the girl.
3:25 p.m.
Rattai arrives in Med Inn Infusion just as Friesen returns from lunch in the University Hospital Cafeteria. Rattai escorts Friesen back to a private room, where she confirms her name and birth date before affixing a wristband.
4:16 p.m.
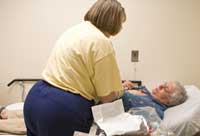
Lynn Lamirand numbs the area around the port in Friesen's chest -- a device implanted under the skin that allows easy access to a vein. Then nurse Theresa Sirrine administers two anti-nausea drugs. She checks the calculations on the doctor's order and the pharmacy's label. "Perfect," she says, continuing to scan the results of Friesen's blood work.
4:48 p.m.

Sirrine returns with Maria Armstrong-Anderson, another infusion nurse, to check the calculations again as well as the calibrations. Because Friesen's infusion takes 24 hours, a home nurse will disconnect the infusion at the end of her treatment.
5:01 p.m.
Friesen leaves the clinic and heads for home.
Continue reading the Fall, 2007 issue of Thrive.
